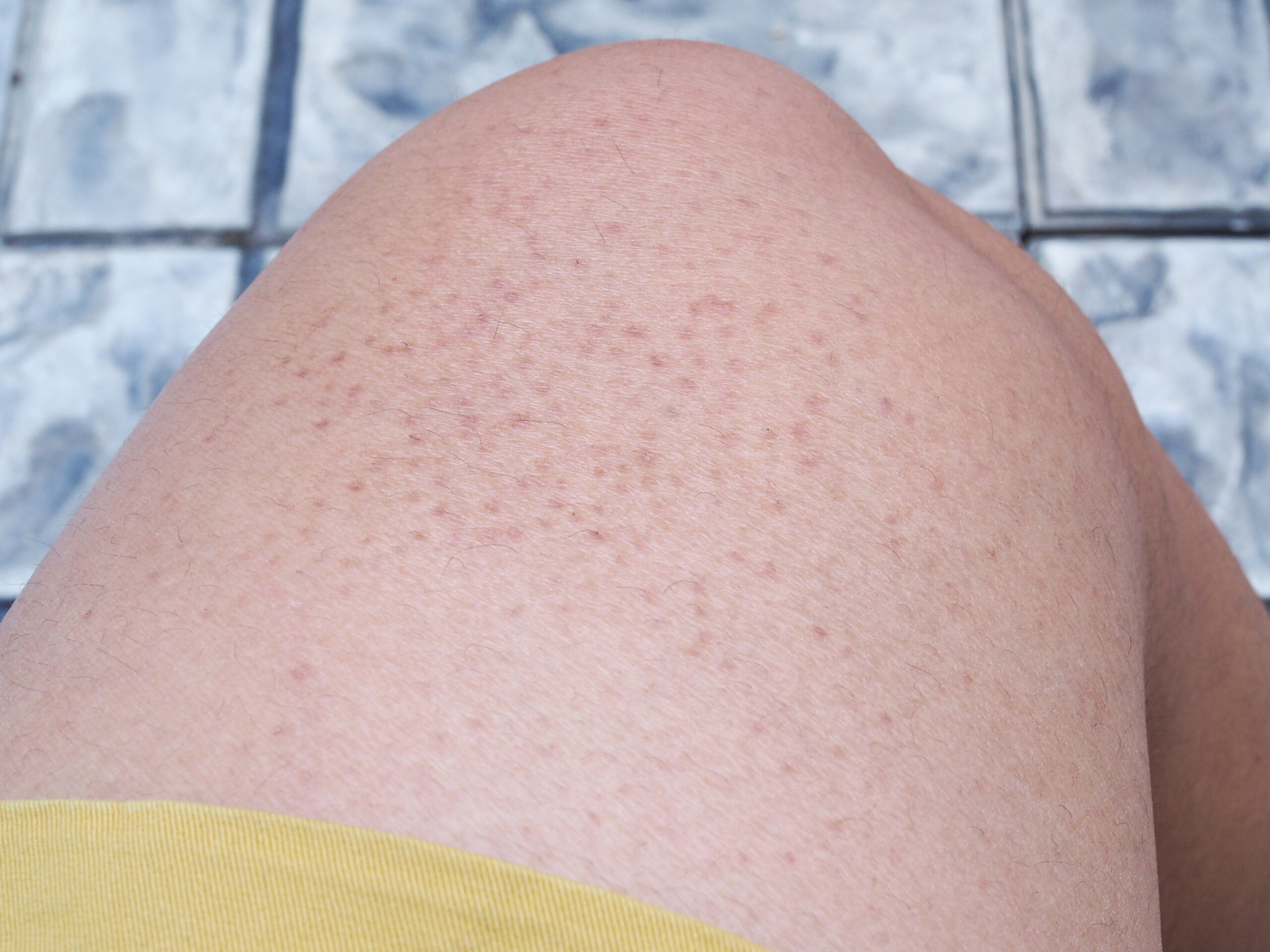
Does Gluten Cause Keratosis Pilaris (a.k.a. Chicken Skin)?
By Amy Burkhart, MD, RD | Dr. Burkhart is the only physician in the United States who is also a registered dietitian and board-certified in integrative medicine.
Chicken skin is a term commonly used for the skin condition keratosis pilaris. According to “Dr. Google,” this rash on the backs of arms, cheeks, and thighs is made worse by eating gluten. Can cutting gluten from the diet help? Is there truth to this claim, or is it another internet myth?
This rash is seen in up to 50% of the world’s population. These tiny bumps can be cosmetically unappealing but don’t cause other symptoms or harm. They can be emotionally distressing for some, especially at times of flare-ups.
My patients often ask me what causes these bumps. Is it a gluten rash? Are there other diet changes that help? How can I get rid of it?
Keratosis Pilaris Explained
It is associated with other inflammatory conditions such as allergies and asthma
Keratosis pilaris ( aka chicken skin rash or KP) occurs due to overproduction or build-up of keratin, a protective protein found on the skin. The bumps can be surrounded by redness, a sign of inflammation seen when they are looked at under a microscope.
Keratosis pilaris occurs more often in people with eczema or dry skin and worsens in cold or dry weather.
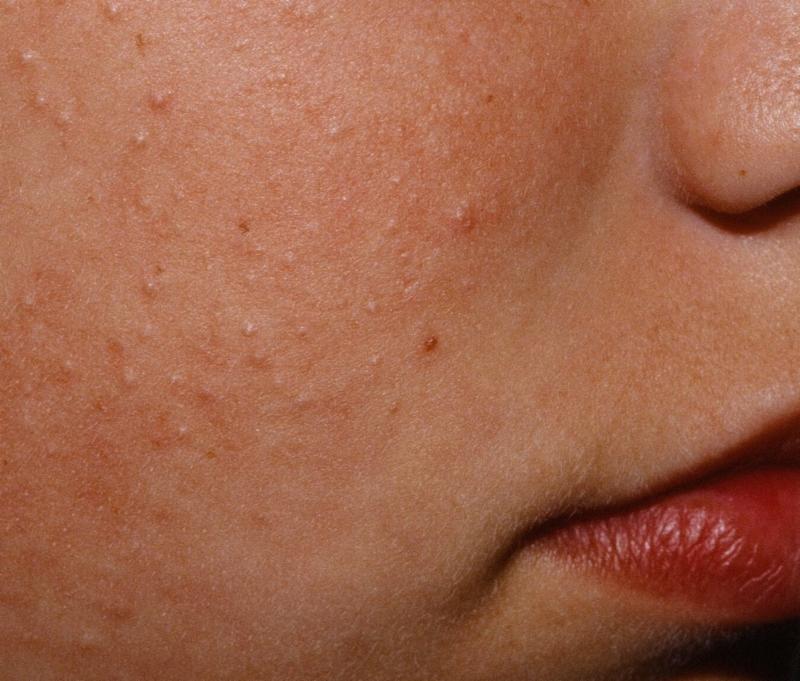
Kids And Adults Get It
Keratosis pilaris affects 50-80% of adolescents and up to 40% of adults.
- It may flare during puberty and decrease with age.
- There is a strong genetic component, so it often runs in families. Symptoms typically come and go throughout the year. Picking at the bumps will only make them more visible and increase scarring and discoloration.
Amy Burkhart MD RD
Causes of Keratosis Pilaris
Although it is known to have a genetic factor, scientists do not know the true cause of keratosis pilaris.
Flares and remissions may occur with hormonal changes such as pregnancy.
Keratosis Pilaris And Gluten
There are no studies indicating a direct correlation between gluten and keratosis pilaris ( chicken skin).
However, it can be caused by vitamin A deficiency or essential fatty acid deficiency, both of which can occur with gastrointestinal absorption problems.
If you have celiac disease or gluten sensitivity you are at risk of poor absorption. In theory, this could increase your odds of having keratosis pilaris due to these nutrient deficiencies.
Amy Burkhart MD RD
Keratosis Pilaris And Diet
Aside from associations with low vitamin A or low essential fatty acid levels, few studies have shown a correlation between diet and keratosis pilaris. Increasing essential fatty acid intake by consuming more coldwater fish such as sardines, mackerel, and salmon may lessen the rash. Walnuts are a great vegan source of essential fatty acids.
Some people say cutting out dairy or sugar has improved their rash. In general, following an anti-inflammatory diet may be beneficial and is not harmful, but there are no studies showing that it improves keratosis pilaris.
Amy Burkhart MD RD
Hydration

Mild cases can be treated with over-the-counter lubricating creams. There is a laundry list of dermatologic therapies such as alpha-hydroxy creams, retinoic acid therapies, and steroids. Dermatologists may prescribe personalized therapies that can be formulated.
Further information on specific medications is beyond the scope of this article but can be found here. For more severe cases, laser therapy and dermabrasion may be used.
Alternative Treatments

The most common alternative treatment for a ” chicken skin rash ” are omega-3 fatty acids ( fish oil supplements).
In addition to providing the essential fatty acids that may be lacking, these supplements also have a strong anti-inflammatory effect.
Dietary manipulations such as gluten-free or dairy-free, anti-inflammatory, sugar-free, Paleo, or various autoimmune diet protocols are often implemented. A variety of ‘gut healing’ regimens are also prescribed, but as with most therapies surrounding keratosis pilaris, there is no evidence to support or refute them.
Topical therapies may include coconut oil, olive oil or vitamin A capsules. Finally, exfoliants such as baking soda, oatmeal, or sugar or salt scrubs are sometimes helpful in reducing keratin build-up. Most people do not seek treatment for keratosis pilaris unless it is cosmetically significant, so home therapies are a popular approach.

Gluten And Keratosis Pilaris Summary
- Although I have seen patients in my office improve their “chicken skin rash’ with gluten elimination, there is no evidence that everyone who suffers from it would benefit by avoiding gluten.
- It would be interesting to see a study exploring a correlation between gluten and keratosis pilaris. But, since there are no known long-term health consequences associated with it, research funding may be a low priority.
- If someone has been appropriately tested for celiac disease, a trial of a gluten-free diet is harmless as long as adequate nutritional intake is maintained.
- Because keratosis pilaris is inflammatory in nature, it also makes sense that anti-inflammatory diet protocols might help KP.
- Lifestyle changes such as stress reduction, mindfulness techniques, and proper sleep hygiene might also improve KP by decreasing inflammation.
- While it is unlikely anyone will be rushing to do those studies soon, there is no reason that you can not implement changes to decrease inflammation on your own. It may just have the additional benefit of improving your keratosis pilaris.