Does Gluten Worsen Pots Syndrome Symptoms?
POTS syndrome and gluten have a connection. But what exactly is POTS syndrome? While it has been recently reported as a long-haul symptom of COVID-19, evidence is also growing that it is an autoimmune disorder. If this is the case, any person with an autoimmune disease would be at increased risk of developing POTS.
POTS (Postural Orthostatic Tachycardia) is a form of dysautonomia. For some people, POTS syndrome symptoms are improved by removing gluten from the diet, a practice that has been validated by research. A 2016 study found people with celiac disease or gluten sensitivity to be at higher risk of POTS/dysautonomia. In my office, I repeatedly see a connection between POTS, celiac disease other gluten-related disorders. Let’s discuss this invisible, life-altering illness, including diet and lifestyle changes that may help people with POTS syndrome feel better.
What Is POTS Syndrome?
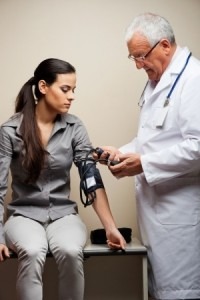
The symptoms of POTS syndrome are often discounted by providers
- POTS occurs when there is dysfunction with the autonomic nervous system.
- This system controls all of the things that happen “automatically” in our body, like blood pressure, heart rate, and breathing.
- POTS is the most common form of dysautonomia/ autonomic disorders.
- Symptoms usually occur or worsen in the upright or standing position. We spend most of our lives upright, so you see how this can significantly impact someone’s life.
- Blood pressure can be low or high (more often low).
- Heart rate abnormalities are frequent but may not be noticed by the person.
- Symptoms may be mild, such as lightheadedness or fatigue, or so severe as to cause someone to lose consciousness.
- Symptoms often improve with hydration, age, and pregnancy.
- Women with POTS often say, “pregnancy was the best I ever felt.”This may be due to the increase in blood volume that occurs in pregnancy, i.e., “the tank is more full.”
People with POTS are commonly misdiagnosed with other conditions, such as chronic fatigue syndrome, fibromyalgia, anxiety, or ADD. They appear outwardly normal and healthy and can experience years of frustration from medical professionals who attribute their symptoms to various maladies or psychological issues.
Symptoms of POTS
Symptoms typically come and go. People with POTS have good and bad days
People with POTS may experience one or many of the following symptoms::
- Symptoms worsen after prolonged periods of standing or sitting, in warm environments, and after eating. They are triggered by dehydration, stress, and exercise.
- A fast heart rate that goes up with standing
- Dizzy or lightheaded
- Palpitations/irregular heartbeat
- Fatigue
- Brain fog/Cloudy thinking
- Weakness
- Headache
- Anxiety
- Shortness of breath
- Nausea
- Digestive symptoms- such as constipation or gastroparesis
- Balance problems
- Muscle pain
- Cold hands and feet
- Exercise intolerance- fatigue with mild exercise
- Pelvic congestion syndrome
- Discoloration or mottling of legs with standing upright*
- Muscle twitching
- *This list is not all-inclusinve

Related Article: A Low Histamine Diet Can Help POTS syndrome symptoms
Is POTS An Autoimmune Condition?
A research paper discusses the possibility of POTS being autoimmune in nature. If POTS is autoimmune, it may be more common in people with other autoimmune diseases such as celiac disease. I am not suggesting that celiac disease or gluten sensitivity is the cause of all cases of POTS. They may be two of several possible reasons for it to occur.
POTS syndrome is challenging for both patients and clinicians. There are treatment centers at several major universities (see list below) dedicated to treating POTS and related autonomic (nervous system) disorders. There is a discussion amongst experts that POTS may be a common endpoint for a variety of illnesses. Thoughts are it may explain many cases of chronic fatigue syndrome.
Related Article: POTS AND COVID- How Are They Connected?
Diagnosing POTS Syndrome
The first step in diagnosing POTS syndrome is considering it as a diagnosis.
Many providers are not familiar with POTS syndrome. It is now more in the headlines due to the correlation with COVID-19. It is being seen as a long-haul symptom of COVID-19.
A diagnosis is made when symptoms occur in conjunction with an increase in heart rate of 30 beats per minute after standing upright for 10 minutes or if the heart rate increases to 120 beats/while standing. Tilt table tests are often done but not at all POTS centers. Other possible medical conditions, such as dehydration, thyroid disease, and adrenal insufficiency, must be ruled out before the POTS diagnosis is made.
POTS syndrome is challenging for both patients and clinicians. There are treatment centers at several major universities (see list below) dedicated to treating POTS and related autonomic (nervous system) disorders. There is a discussion amongst experts that POTS may be a common endpoint for a variety of illnesses. Thoughts are it may explain many cases of chronic fatigue syndrome.

Associated Medical Conditions
Ehler’s Danlos and MCAS are associated with POTS
It is estimated that about 50% of people diagnosed with POTS have hypermobile joints. There may be a connection between Ehler’s Danlos Syndrome and POTS. It is common for POTS to run in families, and there is most likely a genetic component. Many people describe the onset of symptoms after a viral illness (mononucleosis is a common trigger), pregnancy, or trauma. Most of the time, however, cause the cause is unknown.
It is also seen in people with mast cell disorders including MCAS.
Related Article Here- Mast Cell Activation Syndrome (MCAS) : What is it?
Real Life Stories
The impact of POTS syndrome on a person’s life can be severe
To show you the significant effect POTS can have on someone’s life; I wanted to share some stories. These patients* of mine all had either celiac disease or gluten sensitivity. All were all eventually diagnosed with POTS.
Adeline was so tired that at the age of 12, she didn’t have the energy to run around a baseball field during PE. The fatigue was affecting her concentration, grades, and life. Getting to school was a struggle. Making it through, nearly impossible. Jace, 17, was experiencing dizziness and palpitations when he stood for more than a few minutes. His legs ached when he stood. Showers made his pain worse. Standing in line was intolerable. His legs turned a purplish color, and he became exhausted when he stood. He had to sit down frequently. Claire, 35, had headaches that didn’t respond to multiple treatments. Hot weather made them worse. Ruby, 37, suffered from constant brain fog. Her blood pressure “ran low.” Her doctor told her this was “healthy.” She felt awful. Despite the wide range of ages and symptoms, these patients of mine* are connected by one common factor-POTS. *Names are changed for privacy.
POTS Syndrome: The Gluten-Connection

Gluten can make POTS symptoms worse
A paper evaluated a connection between documented celiac disease and autonomic dysfunction. In the study, 2.4% of the patients with autonomic dysfunction had biopsy-proven celiac disease. This is more than double the rate of celiac disease in the general population. A 2016 paper showed POTS patients to be at increased risk for celiac disease and gluten sensitivity. Another study showed 56% of celiac patients had some abnormality in their autonomic nervous system. Should we be considering celiac disease or gluten sensitivity in all patients with POTS? Will removing gluten from the diet improve the symptoms of POTS? In my patients, it improved symptoms, but not completely. Are there cases where it might eliminate POTS symptoms? Does the altered microbiome in celiac disease create symptoms consistent with POTS? If so, could probiotics be of assistance in POTS? Could other food sensitivities, commonly seen with celiac disease, play a role? If future research answers questions such as these, the result could impact many patients.
Treatment Of POTS Syndrome
DIet, water, and lifestyle changes can significantly improve symptoms.
The following lifestyle and dietary modifications can be useful for managing POTS. Prescription medications may be needed in addition to lifestyle changes, but their use is beyond the scope of this article.
Water And Food
Proper hydration is at the forefront of treatment. At least 2 liters of water are recommended daily. Adequate salt intake is also important, and 3-5 grams/day is suggested if someone suffers from POTS. Often salt tablets are used to increase salt intake and help maintain fluid status. Dietary changes also cannot be ignored in the treatment of POTS. Small frequent meals minimize symptoms that may occur after eating. Removing dairy from the diet may be helpful. Decreasing total daily carbohydrate intake is often helpful (Mathias, CJ Other Autonomic Disorders, National Dysautonomia Patient Conference May 2000). Caffeine may be helpful to some POTS patients and worsen symptoms in others. The link between gluten and POTs is emerging, but I hope future studies will evaluate the connection further. I have also anecdotally seen improvement with POTS by removing other food items such as eggs and yeast. Still, these are on an individual basis and can only be determined with an elimination diet. Further research into the effect of particular foods would be interesting, as would manipulating the microbiome with probiotics.

Lifestyle Modifications
- Hydration
- Avoid prolonged sitting or standing
- Avoid warm environments
- Minimize medications that dilate blood vessels
- Assure adequate salt intake
- Avoid alcohol-it worsens symptoms
- Use pressure garments, such as support hose
- Assure adequate, regular sleep. Elevate the head of the bed while sleeping.
- Avoid stressful situations as much as possible
Exercise
Exercise is a cornerstone of long-term improvement. Often at the beginning of treatment, patients go to physical therapy to improve tolerance of exercise. In the beginning, only 1-2 minutes of exercise may be tolerated. It is important to use lifestyle modifications and, if necessary, supplements or medications to bridge the treatment to increase exercise tolerance. The goal is to increase exercise and decrease medication gradually. Long term, exercise helps maintain the vascular tone and minimize symptoms. It often allows discontinuation or minimization of medication.

Posture Adjustments
- Sit in a lower chair or with knees in a knee-chest position
- Squat rather than stand if possible
- Stand with legs crossed and contract muscles while standing
- Bend forward when possible, for example, on a shopping cart if shopping
Treat Associated Conditions
Certain conditions such as asthma, food intolerances, pain, pelvic congestion, anxiety, migraines, and infections can worsen POTS symptoms. They should be addressed immediately if they occur.
Medications
Many medications are used in POTS treatment and include those that increase blood volume, are stimulants, or improve vasoconstriction. The specifics of the medications and their use are beyond the scope of this article. For more information on medications, click here
Vitamins And Supplements
Several supplements have been used as adjunctive treatment to lifestyle modifications. These should only be used under the guidance of your treating physician. They may include butcher’s broom, magnesium, licorice root, magnesium, potassium magnesium, carnitine, and Co-Q10 and adrenal supplements.
Decrease Stress
Because stress exacerbates symptoms of POTS, the use of a daily relaxation technique is beneficial. Possibilities include meditation, journaling, yoga, tai chi, and breathing or muscle relaxation exercises.
Related Article Here- A New Scientific Reason For Food Intolerances
POTS Syndrome: Awareness Is The First Step

The first step in diagnosing POTS is thinking of it as a possibility
After patients understand what they need to do, they can begin to approach it strategically. Regarding my patients above, Adeline participates actively in PE and exercises daily to help her symptoms. She cannot 100% physically keep up with her peers, but she is closer than she has ever been. Her concentration and focus have greatly improved, and her mood is drastically better. Jace can stand now for longer periods of time and is back to playing soccer. His legs no longer ache in the shower, and his mood is markedly better, as is his overall outlook on life. Clare rarely has headaches any longer, and if she does, there is usually a clear trigger. Simply knowing what she is dealing with has helped greatly with her overall situation. She can now manage and modify lifestyle changes as needed to control her symptoms. Rudi is doing better; medications and lifestyle changes have helped alleviate many symptoms.
You may have never heard of POTS before today, but perhaps you know someone who struggles with some of the described symptoms and is searching for answers. POTS might be a possibility, and this information may be life-changing for them. I hope this article will contribute some momentum to further research on a possible link between POTS and diet as well as other treatment options for this challenging illness.
* All names in this article have been changed for privacy
Resources
National Institutes of Health
John’s Hopkins Chronic Fatigue Clinic PDF by Dr. Peter Rowe with additional resources
Dysautonomia information network – Patient Support Network
Dysautonomia International
Dysautonomia Youth Network of America
Research On POTS And Gluten
- Disturbances of autonomic nervous system activity and diminished response to stress in patients with celiac disease
- Autonomic imbalance in celiac children
- Autonomic neuropathy and coeliac disease
- Autonomic dysfunction and upper digestive functional disorders in untreated adult coeliac disease





